Synergy Between Two Types of De-worming Drugs Found Promising in a Lab Test
MARCH 15, 2010
By: Susan Brown

Yan Hu found that when roundworms develop resistance to one type of drug, they become more vulnerable to a second type.
A new combination drug treatment for parasitic intestinal roundworms shows promise in a test on a common laboratory species.
Several drugs currently in use or in development control parasitic worms in the same way. That concerns health workers in developing countries where reinfestations often require repeated treatments. If worms develop resistance to one drug, the other treatments would likely fail as well.
Raffi Aroian's research group at the University of California, San Diego recently demonstrated that a potential new drug, a protein crystal made by bacteria that works by a different mechanism, will rid laboratory animals of intestinal worms. This week, they report that combining these two types of anti-worm treatments could head off the development of drug resistance and save money by allowing lower doses of both drugs to be used. Their paper appears in the early online edition of the Proceedings of the National Academy of Sciences.
Worms that had become resistant to tribendimidine and similar drugs succumbed to lower doses of the crystal protein, the researchers found. "What was amazing was that we found the converse was also true. When the worms develop resistance to the crystal protein, they become more susceptible to the other class of drugs," said Aroian, a professor of biology at UC San Diego.

Crystal proteins isolated from the bacterium Bacillus thuringiensis are a promising new treatment for intestinal parasites.
Credit: Jim Buckman via Wikimedia Commons
When they exposed worms to both classes of drugs simultaneously, lower doses of each were required to halt their reproduction or growth, or to kill adults. "You can actually reduce the amount of each drug that you use," Aroian said, which will reduce the chance of harmful side effects and lower costs. Combining drugs will also help to prevent drug resistance. "The worms would have to mutate two different things simultaneously to resist the combination therapy," he said.
Aroian's group tested the drugs on C. elegans, a common laboratory species. Because all known effective treatments for parasitic worms also kill C. elegans, this free-living soil nematode should be a good stand-in for the parasites, Aroian said. His lab has already begun to test the dual treatment on parasitic worms maintained in culture dishes and plans additional experiments with small animals infested with parasitic roundworms.
The crystal proteins, derived from a bacterium called Bt, are thought to be harmless to humans and other vertebrate animals. Although organic farmers have used them as pest controls for decades, Bt toxins will need to be tested for safety and effectiveness in clinical trials before they are approved for medical use.
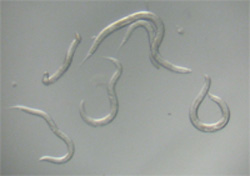
The roundworm C. elegans is a good laboratory stand-in for parasitic species, which can’t be propagated in culture.
The need for those trials is urgent, Aroian said. A recent study found that the drugs did a poor job of ridding school children living in Tanzania of intestinal parasites, evidence that the worms there are developing resistance to currently available treatments.
Although intestinal parasites damage health and mental functioning in ways that keep people poor, the world has made little investment in treating them. The George Institute for International Health, a non-profit organization based in Australia, estimates in a recent report that only $721 thousand dollars was spent worldwide in 2008 to develop treatments for intestinal parasites.
Yet with adequate funding, Aroian thinks the solutions are within reach. "We can do this," he said. "This is an enormous problem that we can solve."
Co-authors on the study include Yan Hu and Audrey Bellier in Aroian's group, and Edward Platzer at the University of California, Riverside. The National Institute of Allergy and Infectious Diseases funded the work.
Related Links